Items filtered by date: December 2021
The Pain in Your Ankle May Be Arthritis
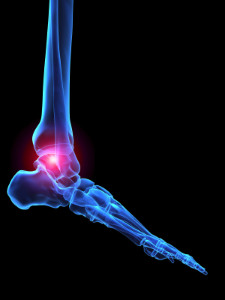 When you feel pain and swelling in the ankle that is not the direct result of an injury, it is likely caused by inflammatory, rheumatoid or crystal arthritis (gout). This condition can also be brought on as a side effect of a previously broken ankle or recurring ankle sprains from sports activities. Other symptoms include reduced mobility and a grinding noise when you move the joint. The main cause is a lack of cartilage, resulting in bone touching bone when you put any weight on your ankle. It may help to use a cane or other device, to take some of the weight off your lower extremities when you stand or walk. In addition, taking anti-inflammatory medication can help to reduce the pain. Wearing a brace to limit joint movement can also be effective. If the pain in your ankle continues or worsens, it is probably wise to make an appointment with a podiatrist, who can fully examine your ankle and offer other treatment options, depending on the severity of the arthritis.
When you feel pain and swelling in the ankle that is not the direct result of an injury, it is likely caused by inflammatory, rheumatoid or crystal arthritis (gout). This condition can also be brought on as a side effect of a previously broken ankle or recurring ankle sprains from sports activities. Other symptoms include reduced mobility and a grinding noise when you move the joint. The main cause is a lack of cartilage, resulting in bone touching bone when you put any weight on your ankle. It may help to use a cane or other device, to take some of the weight off your lower extremities when you stand or walk. In addition, taking anti-inflammatory medication can help to reduce the pain. Wearing a brace to limit joint movement can also be effective. If the pain in your ankle continues or worsens, it is probably wise to make an appointment with a podiatrist, who can fully examine your ankle and offer other treatment options, depending on the severity of the arthritis.
Ankle pain can be caused by a number of problems and may be potentially serious. If you have ankle pain, consult with Sarah Urton, DPM from Kitsilano Foot and Ankle Clinic. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendonitis
- Achilles tendon rupture
- Stress fractures
- Bursitis
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions, please feel free to contact our office located in Vancouver, BC . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Why Pain From Plantar Fasciitis Is Worse in the Morning
Plantar fasciitis will affect 1 in 10 people, mostly between the ages of 40-60, or younger if they are runners, athletes or dancers. The plantar fascia is the web-like fibrous tissue connecting the heel bone with the toes on the sole of the feet. Stress, micro-tears or other damage to the plantar fascia can cause it to become inflamed, which results in plantar fasciitis. This inflammation, in turn, causes the plantar fascia to tighten during periods of rest or inactivity and typically produces a sharp, stabbing pain towards the middle of heel, where the plantar fascia attaches to it. Initially, once activity is resumed (after waking in the morning, for example), and the plantar fascia begins to stretch, the pain may subside, but will reoccur later in the day. Contributing factors to plantar fasciitis include obesity, foot structure disorders such as flat feet or high arches, having to stand for prolonged periods, and participating in sporting activities with repetitive stress on the plantar fascia (i.e., running and jogging). If you have heel pain, it is a good idea to make an appointment with a podiatrist who can determine if plantar fasciitis is the cause and create a treatment plan to reduce your pain and help repair the plantar fascia.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Sarah Urton, DPM from Kitsilano Foot and Ankle Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Vancouver, BC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Are Bunions Affecting Your Everyday Life?
Pregnancy and Foot Health
Many pregnant women complain about foot pain while they are expecting. Foot pain can primarily be caused by weight gain and hormonal changes taking place in the body. By understanding how pregnancy impacts the health of a woman's feet, a pregnant woman can take action to keep her feet as healthy and comfortable as possible.
Because a woman's weight changes during pregnancy, more pressure is brought to bear on both the legs and the feet. This weight shift can cause two major foot problems: over-pronation, also known as flat feet, as well as edema, which is swelling of the feet. Over-pronation occurs when the arch of the foot flattens, causing the foot to roll inwards when the individual is walking, and can aggravate the plantar fascia tissues located along the bottom of the feet. If these tissues become inflamed, a pregnant woman can experience pain in the heel of the foot as well as severe foot pain while walking or standing. Swelling of the feet, or edema, often occurs in the later stages of pregnancy. It is caused by slow circulation and water retention, and may turn the feet a light purple color.
To keep feet in good health and prevent over-pronation, pregnant women should avoid walking barefoot and be sure they are wearing shoes that offer good arch support. A device known as an orthotic can be added to regular footwear in order to provide additional support for the feet during pregnancy. Any expectant mother whose feet hurt should first check to see if the shoes she is wearing are old, worn out and not offering the proper support necessary for distributing the weight of her body during pregnancy.
To treat edema of the feet, a good start is to wear quality footwear which offers support and good circulation. Keep feet elevated whenever possible by using a foot stool while seated. Stay well hydrated by drinking plenty of water to prevent water retention in the feet. Any swelling that occurs in only one foot should be examined as soon as possible by a doctor.
Good foot health during pregnancy can help expectant mothers avoid foot pain that leads to other health problems. Massaging the feet and doing regular gentle exercise like walking aids foot health by contributing to good circulation. Supportive shoes are also a good investment that will support foot health during pregnancy.
Dealing With Swollen Feet During Pregnancy
Many women find that as pregnancy progresses their feet and ankles begin to swell uncomfortably. The main cause of this is a buildup of fluids in the mother that help to support the growing fetus at the same time as her circulation slows down. Symptoms usually occur during the last trimester as the uterus expands, putting more pressure on the legs and feet. This swelling, also known as edema, is usually worse in hot weather and at the end of the day. Among the ways to reduce it are to avoid standing for long periods of time, wear compression stockings, limit salt intake, keep legs elevated on pillows while sleeping, drink lots of water, and do foot exercises to improve circulation. Edema also can be a sign of certain serious health conditions, such as preeclampsia, which may cause high blood pressure and deep vein thrombosis (blood clots). If swelling appears suddenly, is present more in one foot than the other, or does not subside after resting, please do not hesitate to see a podiatrist as soon as possible for a complete exam and diagnosis of your condition.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with Sarah Urton, DPM from Kitsilano Foot and Ankle Clinic. Our doctor will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
- Wearing orthotics can provide extra support for the feet and help distribute weight evenly
- Minimize the amount of time spent walking barefoot
- Wear shoes with good arch support
- Wear shoes that allow for good circulation to the feet
- Elevate feet if you experience swelling
- Massage your feet
- Get regular, light exercise, such as walking, to promote blood circulation to the feet
If you have any questions please feel free to contact our office located in Vancouver, BC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Laser Treatment for Fungal Nails
A new treatment for fungal nails, or onychomycosis, which has grown in popularity in recent years, is laser treatment. Laser treatment involves the use of a laser that kills fungus in the toenail with heat. Laser therapy causes no side effects and does not affect nearby healthy tissue.
Toenail fungus afflicts almost 10 percent of the U.S. population and is more common among the elderly. The most common symptom of toenail fungus is the discoloration and thickening of the nail. The nail can also become brittle and a foul smell may be produced. In rare cases, pain might be present. While it is not a serious condition, it can lead to a perception of disgust amongst those it affects. There are several different fungi that cause fungal infections. These include dermatophyte, yeast, and mold. The most common of these is dermatophyte.
Diagnosis for fungal nails involves a podiatrist utilizing microscopy and fungal cultures. This will allow the doctor to determine whether it is a fungus or another condition, such as lichen planus, psoriasis, nail damage, and onychogryphosis.
Fungus in the nails can be hard to get rid of with over-the-counter drugs. This is due to the nail being hard and protective, with fungus able to slip between the nail bed and plate. Furthermore the slow growth of the nail increases the difficulty of fungus going away. Laser treatment seeks to get around this by directly penetrating through the nail and killing the fungus. The laser is used on each infected nail for a couple of minutes. Patients then typically return several weeks or months later for another laser treatment. During this time the podiatrist will routinely observe the foot and infection. It is also recommended to wear clean socks and shoes and allow the feet to dry and breathe to prevent toenail fungus.
Laser treatment is still a relatively new treatment and not all podiatrists have laser machines. Ask your podiatrist if they do laser treatment for toenail fungus and if it is right for you.
Why Laser Therapy Is Effective in Treating Toenail Fungus
Onychomycosis, or tinea unguium, is a type of fungal infection that can affect fingernails and, more commonly, toenails. If you have a fungal toenail infection your nail may become thickened, brittle, ragged, crumbly, or discolored. Toenails are made up of layers of fibrous keratin, which the fungus can get in between. The fungus can even grow underneath the nail or in the matrix of the nail (where it grows), causing the nail to separate from the toe. Each of these scenarios can make treating toenail fungus challenging when using oral or topical antifungal medicines. Laser therapy treatment to eradicate toenail fungus has become a popular and effective treatment because it can painlessly and accurately target the fungus within the layers, underneath, or in the matrix of the toenail without affecting healthy structures surrounding it. If you have toenail fungus, contact a podiatrist to see if laser treatment is right for you.
Laser treatment can be an effective way to get rid of toenail fungus. If you have any questions about laser treatment, consult with Sarah Urton, DPM from Kitsilano Foot and Ankle Clinic. Our doctor will assess your condition and provide you with quality treatment for fungal nails.
What Are Toenail Fungal Infections?
Onychomycosis, or fungal infection of the nail, is a relatively common and non-serious condition. Around 10 percent of U.S. citizens are afflicted with fungal nails. Common forms of fungus that infect the nail include dermatophytes, yeasts, and molds.
Symptoms of Toenail Fungal Infections Include:
- Nail thickening
- Brittleness of the nail
- Discoloration of the nail
Diagnosis for Fungal Nails
Fungal infections are diagnosed by fungal culture and microscopy. This will rule out any other conditions such as nail trauma, psoriasis, lichen planus, and onychogryphosis.
What Is Laser Treatment?
Laser treatment is a non-invasive, safe, quick, and painless procedure that uses the heat from a laser to kill fungus in the nail. Each infected nail is targeted with a laser for several minutes. The treatment is usually utilized several different times over a select period. During this time, a podiatrist will keep an eye on the infection.
If you have any questions, please feel free to contact our office located in Vancouver, BC . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The Importance of Biomechanics in Podiatry
Biomechanics and its related study deal with the forces that act against the body and affect things like our movement. In podiatry, biomechanics are studied to determine the movement of the ankle, toes, and the foot, as well as the forces that impact them. Podiatrists who train in this specialty are able to effectively diagnose and treat conditions that affect people’s everyday movement.
Regardless of your lifestyle, age, or any other factors, many people experience foot problems throughout their lives. Twists and turns, improper balance, and added weight are just a few of the things that can add stress to the feet. These issues can also limit our bodies’ mobility that we often take for granted. Pain in the feet and ankles can also trickle up towards the lower legs, knees, hip, and even back area. This affects the way you move around on a daily basis.
Biomechanics and its related study deal with forces that act against the body and affect things like our movement. In podiatry, biomechanics are studied to determine the movement of the ankle, toes, and the foot, as well as the forces that impact them. Podiatrists who train in this specialty are able to effectively diagnose and treat conditions that affect people’s everyday movement.
Regardless of your lifestyle, age, or any other factors, many people experience foot problems throughout their lives. Twists and turns, improper balance, and added weight are just a few of the things that can add stress to the feet. These issues can also limit our bodies’ mobility that we often take for granted. Pain in the feet and ankles can also trickle up towards the lower legs, knees, hip, and even back area. This affects the way you move around on a daily basis.
The history of studying biomechanics dates back to ancient Egypt at around 3000 B.C., where evidence of professional foot care has been recorded. Throughout the centuries, advances in technology, science, and an understanding of the human body led to more accurate diagnosis of conditions such as corns for example. In 1974, biomechanics garnered a large audience when Merton Root founded Root Lab to make custom orthotics. He proposed that corrections of certain conditions could be implemented to gain strength and coordination in the area. Due to his research, we still use his basic principle of foot orthotics to this day.
As technology has improved, so have the therapeutic processes that allow us to correct deficiencies in our natural biomechanics. Computers can now provide accurate readings of the forces, movements, and patterns of the foot and lower leg. Critical treatment options can be provided to patients now who suffer from problems that cause their biomechanics to not function naturally. The best results are now possible thanks to 3D modeling and computing technologies that can take readings and also map out what treatment will do to the affected areas.
These advanced corrective methods were able to come to light thanks to an increase in both the technologies surrounding biomechanics and also the knowledge of how they work naturally. For example, shoe orthotics are able to treat walking inabilities by realigning the posture deviations in patients caused by hip or back problems. Understanding foot biomechanics can help improve movement and eliminate pain, stopping further stress to the foot. Speak with your podiatrist if you have any of these problems.
The Five Phases of Walking
A normal stride, or way of walking, includes five distinct phases: Heel-Strike, Support, Toe-Off, Leg Lift, and Swing. In the Heel-Strike phase, the leading foot makes contact with the ground heel first. The rest of the foot then follows suit in the Support phase, contacting the ground while forcing pass through the leg. In the Toe-Off phase, the foot prepares to leave the ground starting with the heel and ending with the toes. Once the foot is off the ground, the lower leg works to raise it during this Leg Lift phase to prepare for the final phase: the Swing phase. In this phase, the raised leg moves in a forward motion, propelling the body forward. There are various foot conditions that can alter this normal pattern of walking, as well as neurological conditions, skeletal deformities, medical conditions, obesity, arthritis, sensory or motor deficiencies, peripheral arterial disease, and more. If you believe your gait is being compromised in some way, make an appointment with a podiatrist who can perform a biomechanical gait analysis and discuss ways to help correct any abnormalities.
If you have any concerns about your feet, contact Sarah Urton, DPM from Kitsilano Foot and Ankle Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
- Biomechanics dates back to the BC era in Egypt where evidence of professional foot care has been recorded.
- In 1974, biomechanics gained a higher profile from the studies of Merton Root, who claimed that by changing or controlling the forces between the ankle and the foot, corrections or conditions could be implemented to gain strength and coordination in the area.
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our office located in Vancouver, BC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.